Key Takeaways:
- Dental bone grafting is essential for restoring jawbone integrity, especially before implant procedures.
- Innovations like 3D-printed scaffolds and bioactive materials are improving graft success rates.
- Understanding the healing process and post-operative care is crucial for optimal recovery.
Understanding Dental Bone Grafting
For anyone considering dental implants or dealing with jawbone deterioration, dental bone grafting has become a critical solution. This advanced procedure is designed to rebuild and restore lost or weakened jawbone, ensuring the long-term stability of dental restorations. Techniques and outcomes have improved significantly in recent years, making dental bone grafting more predictable and effective. Clinics like the Pikos Institute have contributed to this growing field by sharing insights and pioneering best practices.
Dental bone grafting not only helps maintain facial structure but also prepares the jaw for dental implant placement. This restoration is especially beneficial for patients who have suffered tooth loss, gum disease, or trauma that compromised their jawbone. By adding new bone or bone-like material, dental professionals can facilitate the growth of healthy bone tissue and provide a secure foundation for prosthetic teeth that look and function like natural ones.
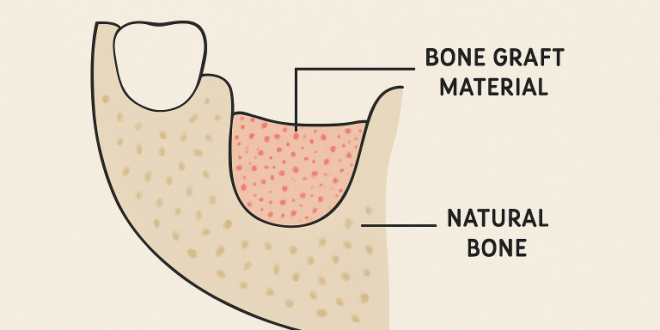
The process relies on carefully selected bone graft materials and techniques tailored to the patient’s specific clinical needs. Successful grafting depends on both the quality of the materials used and the patient’s healing response.
When considering dental bone grafting, it is essential to understand both the biological principles and the technological advancements that have shaped modern treatment options. Staying informed about these changes helps patients make knowledgeable choices about their oral health care.
Types of Bone Graft Materials
Several types of materials are available for bone grafting procedures, and the choice can significantly influence the surgical outcome:
- Autografts: These use bone harvested from the patient’s own body, often from areas like the chin, hip, or tibia. Autografts are valued for their high compatibility and lower risk of immune rejection.
- Allografts: These grafts are sourced from human donors, typically processed and sterilized for safe use. Allografts offer the convenience of avoiding a secondary surgical site but may carry a minimal risk of an immune response.
- Xenografts: Typically derived from animal sources such as cows or pigs, xenografts are carefully processed to be biocompatible. These are often used for their scaffolding properties, which encourage the patient’s natural bone to grow into and replace the graft over time.
- Alloplasts: These are synthetic materials designed to mimic the properties of natural bone. Alloplasts are customizable and eliminate any risk of disease transmission, becoming more common as manufacturing techniques improve.
Dental professionals select the most suitable material based on their patients’ medical history, treatment goals, and the amount of bone needed. Collaboration with specialized centers ensures that patients receive high-quality materials and customized care plans.
Innovations in Bone Grafting Techniques
Recent years have seen notable breakthroughs in dental bone grafting. One of the most exciting advances is the creation of scaffold materials that mimic the microscopic structure of human bone. For example, researchers at the University of Michigan have developed scaffolds with collagen-like nanostructures. These not only provide a framework for new bone cells but also enhance healing by fostering better cellular interactions and accelerating regeneration. Studies have shown these scaffolds can regenerate significantly more bone tissue than traditional materials, representing a major leap forward in grafting success rates.
The Role of 3D Printing in Bone Grafting
3D printing technology has further transformed bone grafting by enabling the fabrication of patient-specific scaffolds. Researchers at the University of Queensland have used 3D-printed resorbable polycaprolactone (PCL) scaffolds customized to the patient’s unique anatomy. These scaffolds are designed to be absorbed by the body over time, simultaneously supporting bone growth and eliminating the need for a second surgery to remove non-resorbable material. Clinical trials have shown improved bone healing, accelerated recovery, and greater implant stability when using these cutting-edge scaffolds.
Healing Process and Post-Operative Care
The healing timeline after dental bone grafting varies depending on the patient’s overall health and the extent of the graft. Generally, initial tissue healing occurs within a week, but complete integration of grafted material with existing bone can take several months. In the days following surgery, patients are likely to experience minor swelling, discomfort, or bruising; these symptoms are typically manageable with prescribed or over-the-counter medication. Following best practices for oral hygiene and strictly adhering to post-operative care instructions is essential for graft success.
Most dental professionals advise regular follow-up visits to monitor healing and make any necessary adjustments to the care plan. Approaches to oral hygiene, diet, and lifestyle modifications may all contribute to optimal recovery and long-term results.
Potential Risks and Complications
Dental bone grafting is considered a safe procedure, but it carries risks, as with any surgical intervention. Possible complications include infection at the graft site, nerve disturbance, or, in rare cases, graft rejection. Working with a highly trained specialist and attending all scheduled post-operative visits can mitigate these risks and ensure early detection of any issues. Detailed guidance on managing pain, recognizing warning signs, and properly caring for the surgical site is important for reducing complications. Comprehensive risk management is a standard part of patient care at all reputable dental centers.
Future Directions in Bone Grafting
The landscape of dental bone grafting continues to evolve as new materials and regenerative medicine concepts emerge. Research is particularly focused on bioactive glass composites and scaffolds infused with growth factors. These innovations have the potential to shorten healing times and further improve graft integration. Looking ahead, ongoing exploration into stem cell therapy and tissue-engineered grafts holds considerable promise for expanding treatment options and enhancing patient comfort and outcomes. Keeping pace with the latest advancements ensures patients benefit from the safest and most effective therapies available.
Final Thoughts
In summary, dental bone grafting plays a vital role in modern restorative dentistry. With ongoing technological improvements and rigorous research, this procedure offers renewed hope to patients seeking to restore oral function and aesthetics. Staying up to date on current trends and consulting experienced professionals can make all the difference in achieving the best possible results.
 Isaiminia World Breaking News & Top Stories
Isaiminia World Breaking News & Top Stories